Swelling of the Feet
There are many reasons why patients experience swelling of the feet. It is rather common and may be a side effect of pregnancy or from sitting and standing for most of the day. Gravity could also play a role in the development of swollen feet. It is known that the weight of blood volume in our bodies is exerted on the veins in the legs and feet. The veins may not work as efficiently during the aging process, and this could make the blood flow backward causing swollen feet. Relief may be found when obese patients lose weight, and it may help to engage in compression therapy by wearing compression socks, stockings, or athletic sleeves. This method can release pressure on the feet and ankles which may help to reduce existing swelling. There are patients who have controlled their swollen feet by implementing healthy lifestyle changes. These can consist of reducing salt intake, incorporating a gentle exercise regime into the daily routine, and drinking plenty of fresh water. Swollen feet may be a temporary condition that affects people who travel via airplane or automobile, so it is beneficial to walk as frequently as possible even though it can be difficult. Swelling of the feet can also be indicative of other health issues so it is important to pay attention to any type of chest pain, mental confusion, dizziness, or fever. If you consistently have swollen feet, it is strongly suggested that you consult with a podiatrist who can help determine the cause and how to effectively treat it.
Understanding and Caring for Diabetic Foot Wounds
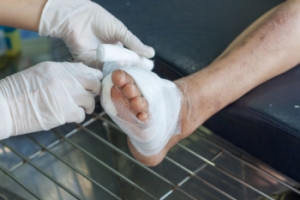
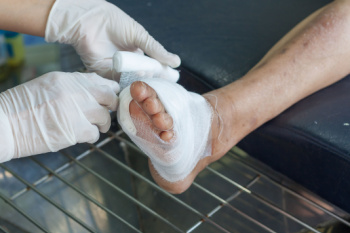 Diabetic foot wounds are common complications resulting from a combination of poor circulation and neuropathy, which reduces sensation in the feet. Risk factors can include prolonged high blood sugar levels, which damage blood vessels and nerves, and wearing ill-fitting shoes, which can cause blisters and sores. People with diabetes are more prone to infections due to a weakened immune response. Proper foot care is essential to prevent these wounds. Daily inspections for cuts, blisters, or any changes in skin color are vital. Keeping feet clean and dry, moisturizing to prevent cracking, and wearing comfortable, protective shoes are essential steps. Regular visits to a podiatrist for foot examinations and managing blood sugar levels effectively can also reduce the risk of severe complications. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this condition.
Diabetic foot wounds are common complications resulting from a combination of poor circulation and neuropathy, which reduces sensation in the feet. Risk factors can include prolonged high blood sugar levels, which damage blood vessels and nerves, and wearing ill-fitting shoes, which can cause blisters and sores. People with diabetes are more prone to infections due to a weakened immune response. Proper foot care is essential to prevent these wounds. Daily inspections for cuts, blisters, or any changes in skin color are vital. Keeping feet clean and dry, moisturizing to prevent cracking, and wearing comfortable, protective shoes are essential steps. Regular visits to a podiatrist for foot examinations and managing blood sugar levels effectively can also reduce the risk of severe complications. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Ingrown Toenail Management
 An ingrown toenail occurs when the edge of a toenail grows into the surrounding skin, causing pain, swelling, and sometimes infection. This condition is often seen in the big toe and can result from improper nail trimming, wearing tight footwear, or injury to the toe. When the nail pierces the skin, it creates an entry point for bacteria, leading to redness, pain, and pus formation. Managing an ingrown toenail involves soaking the affected foot in warm water to reduce swelling, gently lifting the nail edge, and applying antibiotic ointment. It is important to avoid cutting the nail too short or rounding the corners, as this can worsen the condition. Complications from untreated ingrown toenails can include severe infections, abscess formation, and in extreme cases, bone infections. To prevent ingrown toenails, trim nails straight across, wear properly fitting shoes, and maintain good foot hygiene. If the condition persists or worsens, it is suggested that you
An ingrown toenail occurs when the edge of a toenail grows into the surrounding skin, causing pain, swelling, and sometimes infection. This condition is often seen in the big toe and can result from improper nail trimming, wearing tight footwear, or injury to the toe. When the nail pierces the skin, it creates an entry point for bacteria, leading to redness, pain, and pus formation. Managing an ingrown toenail involves soaking the affected foot in warm water to reduce swelling, gently lifting the nail edge, and applying antibiotic ointment. It is important to avoid cutting the nail too short or rounding the corners, as this can worsen the condition. Complications from untreated ingrown toenails can include severe infections, abscess formation, and in extreme cases, bone infections. To prevent ingrown toenails, trim nails straight across, wear properly fitting shoes, and maintain good foot hygiene. If the condition persists or worsens, it is suggested that you
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact one of our podiatrists of Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.
Why Live with Pain and Numbness in Your Feet?
Healing Times for a Broken Foot

Patience and proper care are key to a full recovery from a broken foot. Healing times can vary depending on the location and severity of the break, as well as the patient's overall health and age. Typically, bones take several weeks to mend, with the initial phase focusing on immobilization to ensure proper alignment. During this time, it is important to avoid putting weight on the injured foot to prevent complications. As the weeks progress, gradual weight-bearing activities may be introduced, guided by a podiatrist. Throughout the healing process, specific stretches and other exercises can play an essential role in restoring strength and flexibility. A consistent and careful approach will support the natural healing process, leading to a stronger and healthier foot. If you have broken your foot, it is suggested that you promptly visit a podiatrist who can guide you toward the correct treatment, which may include a walking boot or a cast.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact one of our podiatrists from Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes, Symptoms, and Treatment for a Broken Foot
The human foot has 26 different bones, and the foot is divided into three parts: the hindfoot, the midfoot, and the forefoot. Each section of the foot is composed of a different amount of bones. For instance, the forefoot is made up of 19 bones. The midfoot is composed of five smaller bones called the navicular, cuboid, and three cuneiform bones. Lastly, the hindfoot is made up of only the talus and the calcaneus. The feet tend to be vulnerable to slipping and twisting; consequently, fractured bones within the foot are common. When a bone gets crushed, bent, twisted, or stretched it may become broken.
Many foot fractures occur through an accident or trauma. More specifically, common causes for broken feet are car accidents, falls, missteps, or overuse. If you have a broken ankle or foot, you may have one or more of the following symptoms: throbbing pain, swelling, bruising, tenderness, deformities, and difficulty walking.
There are some factors that may put you at a higher risk of developing a broken foot. People who participate in high-impact sports are more likely to develop foot fractures because of the stresses, direct blows, and twisting injuries involved in gameplay. Additionally, those who suddenly increase their activity level are more likely to suffer a stress fracture.
Unfortunately, there are different complications that may arise because of a foot fracture. For instance, arthritis may be caused by fractures that extend into the joints. Bone infections are also possible in open fractures due to the bone being exposed to bacteria. However, there are ways you can help prevent yourself from breaking your foot. One way to avoid fractures is to wear proper footwear. If you plan on going on a run, you should wear running shoes. You should also replace your shoes if you notice that they are becoming worn out. For runners, it is best to replace shoes every 300 to 400 miles.
Treatment for foot fractures usually consists of rest, ice, elevation, and compression (RICE). If you plan on wrapping your foot, try not to wrap it too tightly because doing so may cut off blood supply in the foot. You should also avoid walking on the fractured foot.
If you suspect you have a broken foot, you should see your podiatrist right away. It is important that you have someone bring you to your doctor, since driving with a broken foot can be dangerous. You should especially seek urgent care if you are experiencing numbness, pain, or deformities in your foot.
What Does Tarsal Tunnel Syndrome Feel Like?
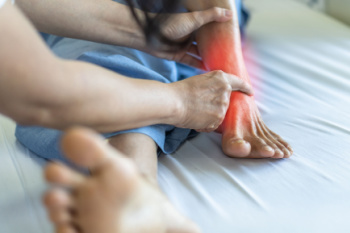 Tarsal tunnel syndrome is caused by compression of the posterior tibial nerve as it passes through the tarsal tunnel, which is a narrow space on the inside of the ankle. This nerve entrapment can result overuse, injury, inflammation, or structural abnormalities, such as flat feet or varicose veins. Symptoms of tarsal tunnel syndrome include tingling, burning, or shooting pain in the foot and ankle, numbness, and a feeling of electric shocks radiating into the sole. These symptoms often worsen with prolonged standing or walking. Diagnosis involves a physical examination, focusing on the areas of pain and nerve compression, in addition to imaging studies like MRI scans or ultrasounds to identify underlying causes. Nerve conduction studies may also be used to assess the function of the posterior tibial nerve. Relief options include rest, anti-inflammatory medications, and exercises to alleviate symptoms. Orthotic devices can help reduce pressure on the nerve, and in severe cases, surgical intervention may be necessary. Complications from untreated tarsal tunnel syndrome can lead to chronic pain and permanent nerve damage. If you have pain in this part of your foot, it is suggested that you schedule an appointment with a podiatrist for a precise diagnosis and individualized treatment plan.
Tarsal tunnel syndrome is caused by compression of the posterior tibial nerve as it passes through the tarsal tunnel, which is a narrow space on the inside of the ankle. This nerve entrapment can result overuse, injury, inflammation, or structural abnormalities, such as flat feet or varicose veins. Symptoms of tarsal tunnel syndrome include tingling, burning, or shooting pain in the foot and ankle, numbness, and a feeling of electric shocks radiating into the sole. These symptoms often worsen with prolonged standing or walking. Diagnosis involves a physical examination, focusing on the areas of pain and nerve compression, in addition to imaging studies like MRI scans or ultrasounds to identify underlying causes. Nerve conduction studies may also be used to assess the function of the posterior tibial nerve. Relief options include rest, anti-inflammatory medications, and exercises to alleviate symptoms. Orthotic devices can help reduce pressure on the nerve, and in severe cases, surgical intervention may be necessary. Complications from untreated tarsal tunnel syndrome can lead to chronic pain and permanent nerve damage. If you have pain in this part of your foot, it is suggested that you schedule an appointment with a podiatrist for a precise diagnosis and individualized treatment plan.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact one of our podiatrists of Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.