What Are Bunions?
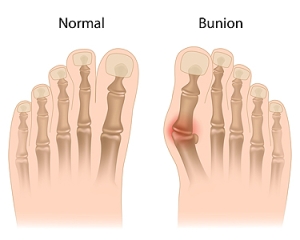
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
Diabetic Foot Care Tips
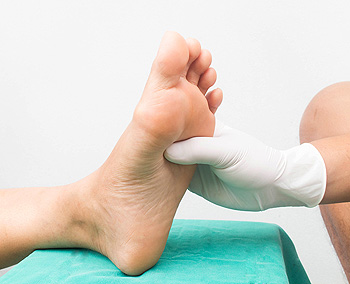 Diabetic patients are at a higher risk for foot related issues. Those with diabetes are more prone to developing poor blood circulation. One common condition, known as neuropathy, which leads to the loss of sensation in the feet, changes in the shape of the feet, and cuts or sores that do not heal properly, is also common among diabetic patients. Because of these potential issues, daily foot care is very important. One key step to foot care is doing daily checks for problems such as cuts, sores and infections. Making sure to regularly wash your feet with warm water and to dry them thoroughly is also suggested. It is also beneficial to always wear shoes and socks in order to protect the feet from extreme temperatures. Keeping up circulation by periodically wiggling the toes and exercising is suggested as well. Lastly, it is important to go to your podiatrist for regular checkups, and to let them know if you are experiencing any foot problems.
Diabetic patients are at a higher risk for foot related issues. Those with diabetes are more prone to developing poor blood circulation. One common condition, known as neuropathy, which leads to the loss of sensation in the feet, changes in the shape of the feet, and cuts or sores that do not heal properly, is also common among diabetic patients. Because of these potential issues, daily foot care is very important. One key step to foot care is doing daily checks for problems such as cuts, sores and infections. Making sure to regularly wash your feet with warm water and to dry them thoroughly is also suggested. It is also beneficial to always wear shoes and socks in order to protect the feet from extreme temperatures. Keeping up circulation by periodically wiggling the toes and exercising is suggested as well. Lastly, it is important to go to your podiatrist for regular checkups, and to let them know if you are experiencing any foot problems.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Care
Diabetes affects millions of people every year. Blood vessels located all over the body are damaged due to diabetes—even the blood vessels of the feet. Neuropathy, or nerve damage, can result from slower blood flow in the legs and feet. In diabetic patients, neuropathy is very important to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care. There should be a focus on cleaning between the toes. Even if no pain is felt, the entire foot should be examined for redness and sores. Neuropathy can often mask the pain of sores and ulcers and can cause these conditions to be overlooked. Use a mirror to examine the underside of your feet if needed. It is recommended that diabetics wear well-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised. It is very important to keep your blood sugar levels in the normal range, which can be determined by your physician. There are medications that may be prescribed to help with any neuropathy experienced by the diabetic patient. It is also advisable to visit a podiatrist if one is experiencing any conditions involving the feet, such as ingrown toenails, which in more severe cases can cause infection.
Diabetic feet must be inspected daily. Diabetic foot care at home is possible if a patient is provided with instructions from their podiatrist. Patients can relieve dry heels with creams or ointments. Suspected wounds should warrant an immediate call to the podiatrist. Gangrene is a serious problem for diabetics and can lead to sepsis and amputation in its worst cases. Early treatment and daily inspection of diabetic feet are keys to staying healthy.
Two Categories of Flat Feet
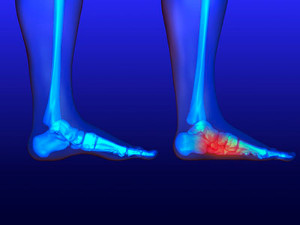 Patients who are missing an arch in their foot have the condition that is known as flat feet. Flat feet fall into two categories. Flexible flat feet have an arch that disappears when the foot bears weight and reappears while sitting or standing on tiptoes. Rigid flat feet do not have an arch regardless of whether you stand or sit. Children that have flat feet may benefit from wearing soft insoles, and this may provide additional comfort. If your child has flat feet that are causing them discomfort, it is suggested that you confer with a podiatrist who can offer treatment options.
Patients who are missing an arch in their foot have the condition that is known as flat feet. Flat feet fall into two categories. Flexible flat feet have an arch that disappears when the foot bears weight and reappears while sitting or standing on tiptoes. Rigid flat feet do not have an arch regardless of whether you stand or sit. Children that have flat feet may benefit from wearing soft insoles, and this may provide additional comfort. If your child has flat feet that are causing them discomfort, it is suggested that you confer with a podiatrist who can offer treatment options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact one of our podiatrists from Summit Podiatry. Our doctors will treat your foot and ankle needs.
What Are Flat Feet?
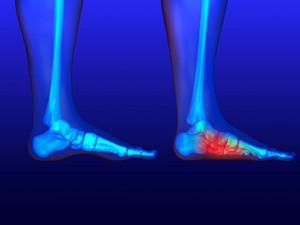
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot
Flatfoot is a foot disorder that is not as straightforward as many people believe. Various types of flatfoot exist, each with their own varying deformities and symptoms. The partial or total collapse of the arch, however, is a characteristic common to all types of flatfoot. Other signs of flatfoot include:
- “Toe drift,” or the pointing outward of the toes and the front part of the foot
- The tilting outward of the heel and the tilting inward of the ankle
- The lifting of the heel off the ground earlier when walking due to a tight Achilles tendon
- Hammertoes
- Bunions
One of the most common types of flatfoot is flexible flatfoot. This variation usually starts in childhood and progresses as one ages into adulthood. Flexible flatfoot presents as a foot that is flat when standing, or weight-bearing. When not standing, the arch returns. Symptoms of flexible flatfoot include:
- Pain located in the heel, arch, ankle, or along the outside of the foot
- Overpronation, or an ankle that rolls in
- Shin splint, or pain along the shin bone
- General foot aches or fatigue
- Pain located in the lower back, hip, or knee
Your podiatrist will most likely diagnose flatfoot by examining your feet when you stand and sit. X-rays may be taken to define the severity and help determine the treatment option best for your condition. Nonsurgical treatments can include activity modification, weight loss, orthotics, immobilization, medications, physical therapy, shoe modifications, and ankle foot orthoses (AFO) devices. If nonsurgical methods prove ineffective, surgery may be considered. Multiple surgical procedures can correct flatfoot; and depending on your specific condition, one may be selected alone or combined with other techniques to ensure optimal results.
What Happens During an Ankle Sprain
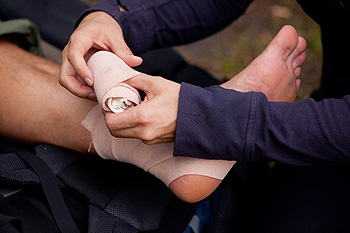 The ligaments in the ankle connect the bones to each other and provide stability to the ankle. When these ligaments are torn or stretched due to an accidental twist or roll of the ankle, a sprain can occur. Ankle sprains are some of the most common injuries that occur in sports that require quick changes in direction such as soccer, football, and basketball. Athletes who have had an ankle sprain before are at a higher risk for developing them again. Patients who believe they may have an ankle sprain should consult with a podiatrist. A podiatrist will examine the ankle and take X-rays to make sure that it is not broken. While most ankle sprains are treated with anti-inflammatory medications, ice, and supportive devices, a podiatrist will be able to determine the right treatment for you.
The ligaments in the ankle connect the bones to each other and provide stability to the ankle. When these ligaments are torn or stretched due to an accidental twist or roll of the ankle, a sprain can occur. Ankle sprains are some of the most common injuries that occur in sports that require quick changes in direction such as soccer, football, and basketball. Athletes who have had an ankle sprain before are at a higher risk for developing them again. Patients who believe they may have an ankle sprain should consult with a podiatrist. A podiatrist will examine the ankle and take X-rays to make sure that it is not broken. While most ankle sprains are treated with anti-inflammatory medications, ice, and supportive devices, a podiatrist will be able to determine the right treatment for you.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact one of our podiatrists from Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle Sprains
Ankle sprains occur when ligaments that support the ankle stretch beyond their limits and tear. These types of injuries are very common and can occur in people of all ages. Sprains may range from mild to severe, depending on how much damage is done to the ligaments. If a sprain goes untreated, a more severe sprain may occur which can further damage the ankle. Repeated ankle sprains can lead to chronic ankle pain.
There are some risk factors that can increase your risk of suffering a sprained ankle. Those who participate in sports, walk on uneven surfaces, have a prior ankle injury, are in poor physical condition, or wear improper shoes are more likely to get a sprained ankle.
There are a few symptoms to look out for if you suspect you are suffering from a sprained ankle. Some common symptoms are swelling, bruising, tenderness, and instability of the ankle. In cases where the tearing of the ligaments is severe, there may be a “popping” sound when the strain occurs.
The RICE method is proven to be effective in treating ankle sprains. RICE stands for Rest, Ice, Compression, and Elevation. Rest is important for treatment, especially within the first 24 to 48 hours. You should also ice your sprained ankle for the first 48 hours for 20 minutes at a time. A small piece of cloth should be placed between the ice and the affected area. For the compression step, you should wear a brace that is snug, but not too tight that it cuts off circulation. When choosing a brace, be sure to choose one that is suitable for the type of ankle sprain you have. Lastly, you should elevate your foot above the heart as often as possible.
After you treat a sprain, you should go through rehabilitation to prevent the injury from occurring again. There are three phases to the rehab process. The first phase involves resting, protecting, and reducing the swelling of the injury. The second phase consists of restoring the ankle’s flexibility, range of motion, and strength. The third phase consists of slowly returning to activity and maintenance exercises.
If you suspect you have an ankle sprain, you shouldn’t hesitate to consult with your podiatrist. Your podiatrist will be able to give you a proper diagnosis and a suitable treatment option for your condition.
Common Reasons a Bunion Can Develop
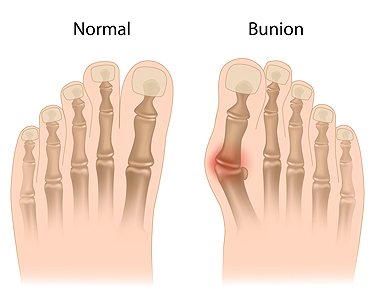 A bunion is a bony protrusion that forms at the base or side of the big toe and can gradually develop for genetic reasons. Additionally, wearing shoes that do not fit correctly may also contribute to the formation of a bunion. It appears as a deformity that can cause pain and discomfort. Some patients find mild relief when a protective pad is worn over the bunion, and it may be necessary to wear orthotics. Additionally, it can help to perform specific stretches that can strengthen the toes and surrounding muscles. If you notice a bunion is developing, it is suggested that you consult with a podiatrist who can offer treatment options, such as surgery for permanent removal.
A bunion is a bony protrusion that forms at the base or side of the big toe and can gradually develop for genetic reasons. Additionally, wearing shoes that do not fit correctly may also contribute to the formation of a bunion. It appears as a deformity that can cause pain and discomfort. Some patients find mild relief when a protective pad is worn over the bunion, and it may be necessary to wear orthotics. Additionally, it can help to perform specific stretches that can strengthen the toes and surrounding muscles. If you notice a bunion is developing, it is suggested that you consult with a podiatrist who can offer treatment options, such as surgery for permanent removal.
If you are suffering from bunions, contact one of our podiatrists of Summit Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Why Does the Ball of My Foot Hurt?
 Metatarsalgia is pain in the ball of the foot, under the base of the toes. The five bones known as the metatarsals connect to the toes and are generally affected by this type of pain. While the pain in the ball of the foot may not be serious and can be aided by rest, ice and properly fitting shoes, it can be an indicator of a variety of foot conditions. Any issues that affect how the foot functions, such as neuromas, bunions, hammertoes, stress fractures, arthritis, or damaged ligaments, can lead to pain in the ball of foot. Therefore, it is suggested to consult with a podiatrist if the pain persists for more than a few days.
Metatarsalgia is pain in the ball of the foot, under the base of the toes. The five bones known as the metatarsals connect to the toes and are generally affected by this type of pain. While the pain in the ball of the foot may not be serious and can be aided by rest, ice and properly fitting shoes, it can be an indicator of a variety of foot conditions. Any issues that affect how the foot functions, such as neuromas, bunions, hammertoes, stress fractures, arthritis, or damaged ligaments, can lead to pain in the ball of foot. Therefore, it is suggested to consult with a podiatrist if the pain persists for more than a few days.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with one of our podiatrists from Summit Podiatry. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Wilmington, Whiteville, and Wallace, NC . We offer the newest diagnostic and treatment technologies for all your foot care needs.